From Patient Event to Cash Collection
In today’s healthcare environment, hospitals face unprecedented challenges. Balancing quality patient care with financial sustainability is more complex than ever. Rising administrative costs, growing regulatory demands, and increased pressure from both public and private payers are squeezing margins. As a result, many healthcare providers are reevaluating the systems that drive one of their most critical operations: billing.
Billing is often seen as a back-office function, but in reality, it is the financial heartbeat of the hospital. From the moment a patient enters the facility to the point at which payment is received, every step in the care delivery process has implications for revenue. Unfortunately, many hospitals still rely on fragmented systems and manual workflows that lead to delays, claim denials, and revenue leakage.
To thrive in this evolving landscape, hospitals must modernize their billing infrastructure. That means connecting clinical and financial data in real time, automating repetitive tasks, and enabling staff to focus on high-value decisions rather than administrative burdens. When done right, billing transformation can reduce errors, improve cash flow, and free up resources to reinvest in patient care.
At the core of this transformation is a robust Revenue Cycle Management (RCM) platform — one that integrates seamlessly with the hospital’s Electronic Medical Record (EMR), financial systems, and insurance ecosystem. With a modern platform like ECH, hospitals can convert patient activity into clean, validated claims that accelerate reimbursement and improve visibility across departments.
Let’s walk through the modern hospital billing process as an end-to-end workflow — from patient encounter to cash collection.
Step 1: Capturing the Clinical Event
Every billing journey begins at the point of care. As a patient receives services — whether it’s a diagnostic test, outpatient procedure, or full inpatient stay — the EMR captures critical information such as:
- Diagnoses and treatments
- Provider details
- Department or location
- Insurance coverage and patient demographics
This clinical event becomes a “billing event,” meaning it contains the raw data needed to calculate charges and submit claims.
Step 2: Connecting EMR Data to the Billing Engine
Instead of waiting until discharge or manually exporting data, a HIS Connector continuously extracts relevant billing data from the EMR in real time or scheduled batches. This includes:
- Service codes (CPT, DRG, ICD-10)
- Units and quantities
- Pricing groups
- Payer-specific contract information
The connector ensures clean handoff of structured data to the billing platform — eliminating transcription errors or data silos that often lead to denials.
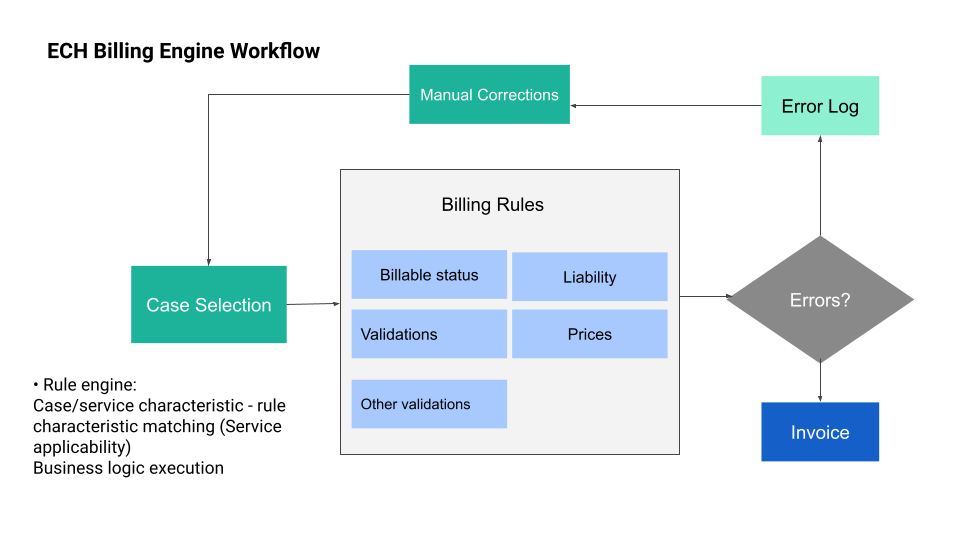
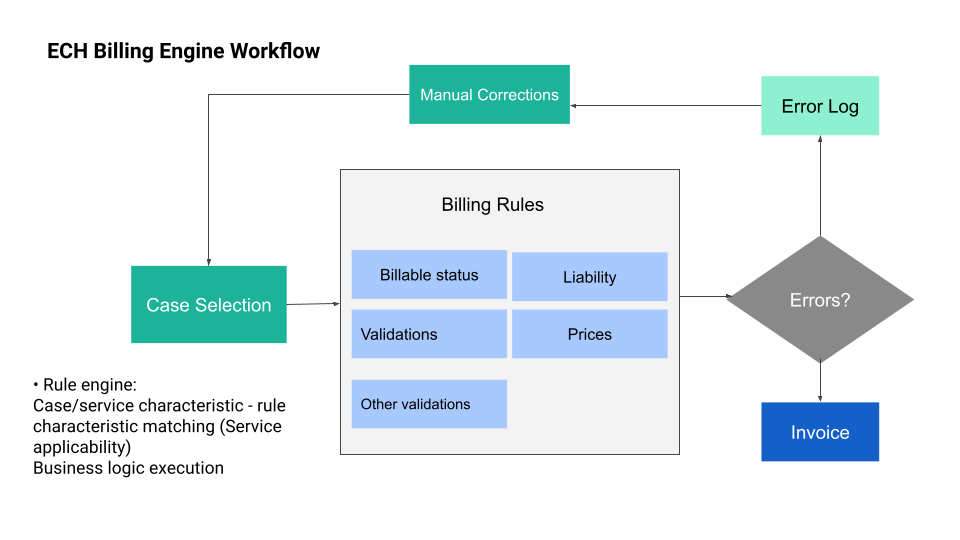
Step 3: Automated Billing Orchestration
Once in the billing platform (like ECH’s Billing Workstation), services are automatically grouped by episode or visit, and business rules are applied:
- Service bundling or unbundling based on payer policy
- Internal coding validation (e.g., missing modifiers, diagnosis mismatches)
- External rules engine (e.g., payer-specific logic, cross-checks)
Clean claims or invoices are automatically generated in the right format — HL7, FHIR, XML, PDF, etc. — ready for electronic submission.
Step 4: Billing Team Oversight via Smart UI
While automation handles the bulk of routine processing, billing staff still play a critical role in resolving edge cases. The platform provides:
- A user-friendly Fiori-based UI to monitor claim status
- Exception dashboards highlighting incomplete or flagged entries
- Real-time alerts to reduce delays
This setup empowers staff to manage by exception rather than sifting through every record manually.
Step 5: Seamless Integration with Finance and Collections
Validated invoices are pushed into SAP S/4HANA ERP, where they trigger downstream financial processes:
- Posting to Accounts Receivable
- Claim status tracking
- Denial management workflows
- Payment reconciliation
The entire revenue cycle is now auditable, traceable, and visible — from front-end services to backend cash flow.
Why a Modern Billing Process Matters
The benefits of an integrated billing process go far beyond faster payments:
- Reduced administrative burden: Automation eliminates repetitive tasks and manual data entry.
- Improved accuracy: Fewer errors mean fewer denied claims and less rework.
- Faster reimbursement: Clean claims are processed quicker, reducing days in A/R.
- Financial visibility: Real-time dashboards help CFOs and revenue managers make informed decisions.
- Better patient experience: Accurate, timely billing reduces confusion and improves satisfaction.
Hospital billing is no longer just about sending out claims — it’s a strategic function that connects patient care to financial outcomes. By modernizing billing workflows with platforms like ECH, hospitals can unlock real operational and financial gains. In a system where every delay has a cost and every inaccuracy creates friction, a smarter, connected billing process ensures that hospitals remain resilient and ready to focus on what they do best: saving lives and serving communities.